Καρδιακή Αποκατάσταση σε Χρόνια Νοσήματα: Από τη Φροντίδα Νεφρών στην Ψηφιακή Καινοτομία
Host (Isabella Marcel): Welcome to this episode of Let’s Talk ICPR podcast season 2. I’m your new host Isabella Marcel and today I’m joined by ICCPR friend Dr. Evangelia Gudy. Thank you so much for being here today. Your research spans exercise in both chronic cardiac populations and kidney disease. What first drew you to explore cardiac rehab in this clinical settings?
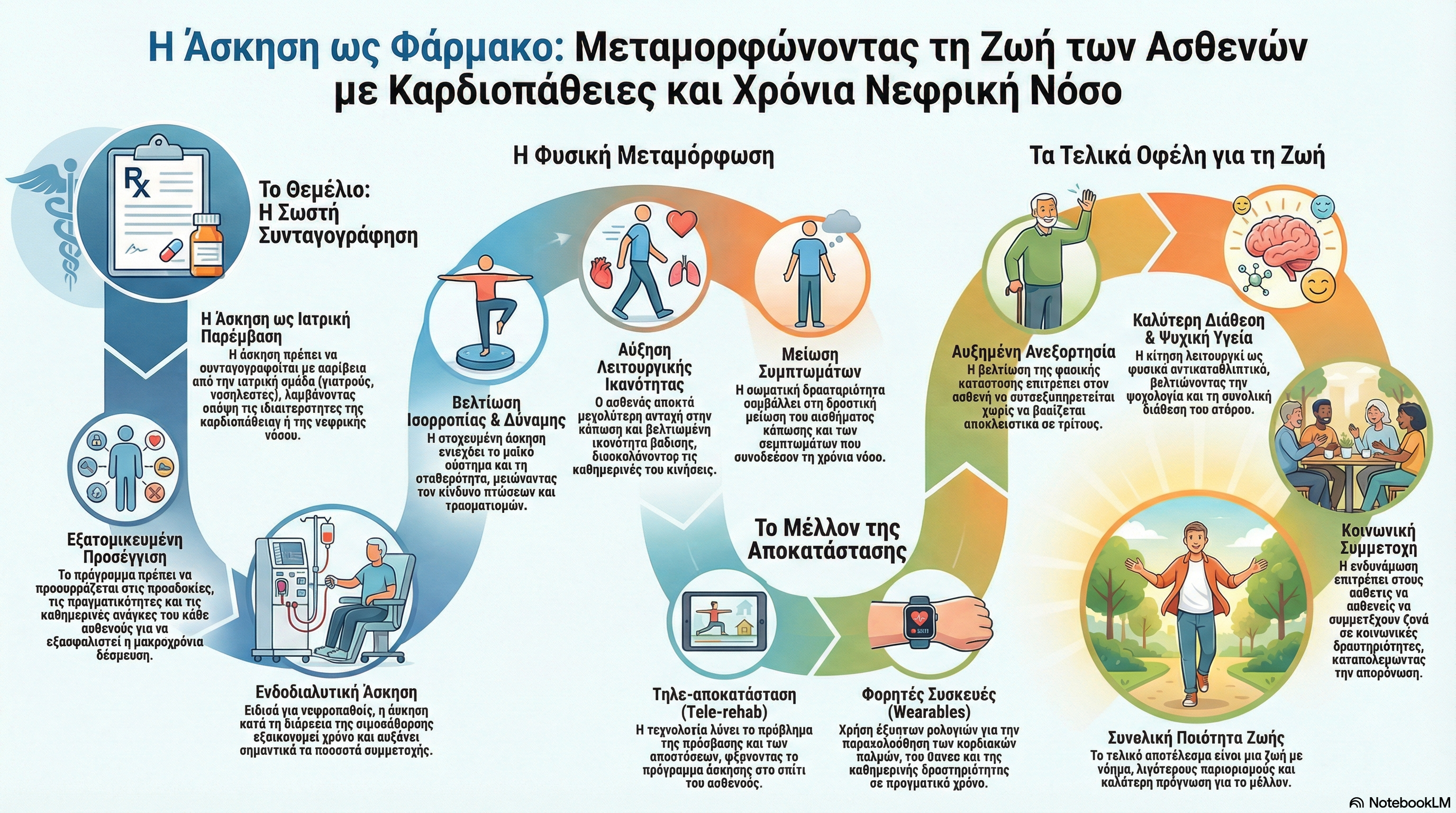
Guest (Dr. Evangelia Gudy): Thank you for the invitation. What first drew me in was the gap between what we can do medically and what patients actually feel every day. So there’s a difference between heart disease and kidney disease. In heart disease, we do know that structured exercise improves functional capacity and prognosis. On the other hand, in chronic kidney disease and especially in dialysis, this patient the symptoms burden is enormous and unfortunately rehabilitation is underused. So we know that in these patients there are many limitations that are treatable and if we perform right exercise prescription even in the very complex patients they can feel better they may have better quality of life and we may decrease fatigue and symptoms and even small improvements in walking, strength, balance can improve their quality of life. It’s very important.
Host: Your research now is focused on patients with chronic disease.
Guest: Yes, both cardiac disease and chronic kidney disease. I’m a cardiologist so cardiac patients and cardiac rehabilitation is my first priority. But patients with chronic kidney disease and other chronic diseases as diabetes, pulmonary diseases also need exercise. So we provide exercise training prescriptions in any kind of patients.
Host: Awesome. And what are the main findings so far? If you can share a little bit about your research and kidney disease.
Guest: If patients can move better, they feel better and they live better if they have gains in balance, functional capacity, strength and tolerance. They have gains in independence, mood, and social participation. That means that they improve their quality of life. So, exercise can be a medication.
Host: Well, thank you. And I also know you were involved in several European projects focused on promoting behavior change in patients with chronic disease overall. So, what have been the most important lessons especially translating these models into real world practicing?
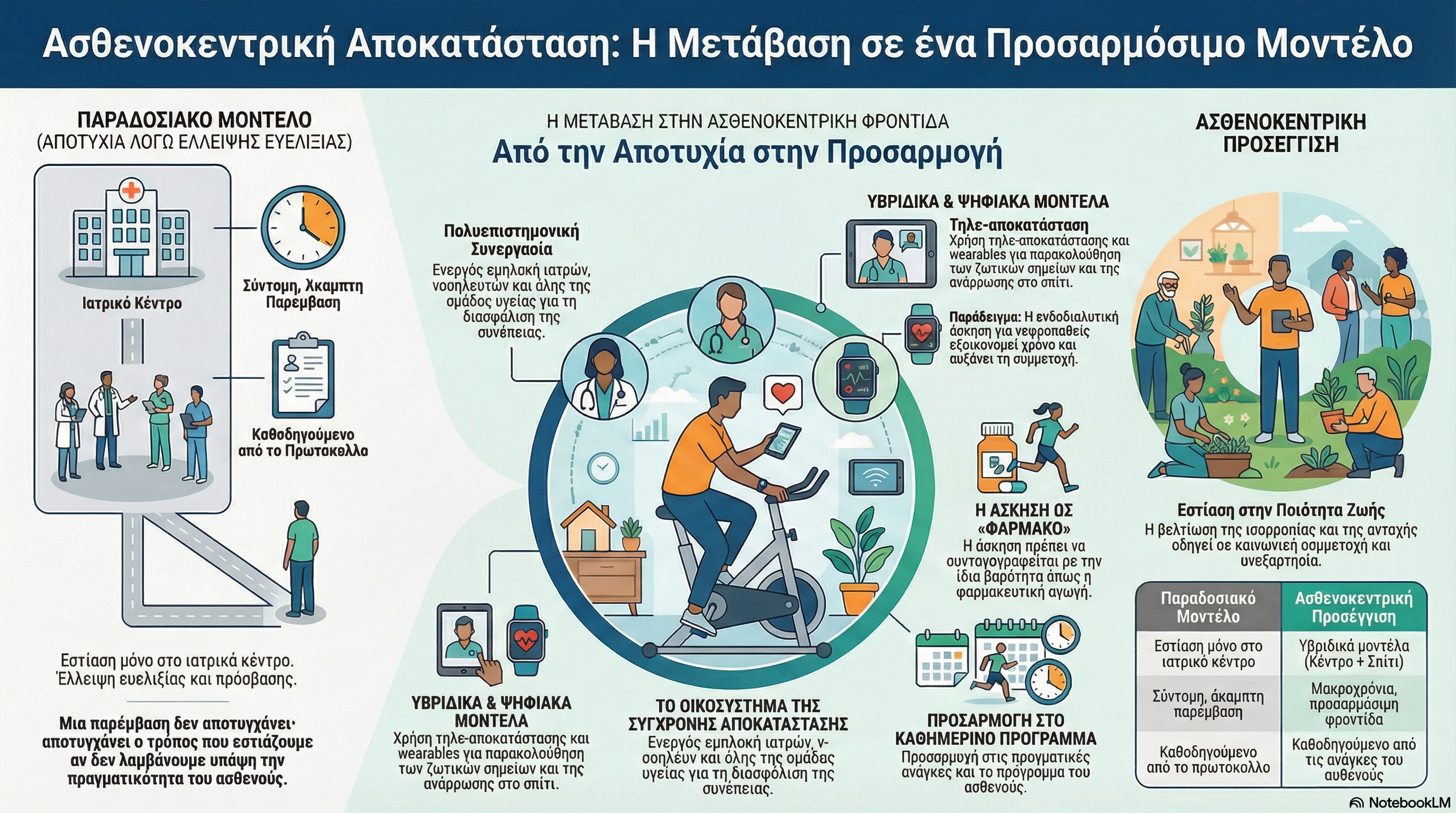
Guest: We should focus on long-term interventions that means that an intervention doesn’t actually fail. The way we focus may fail. We need to focus on the fact that exercise must be prescribed like medication as I said and also it is important physicians, nurses, all healthcare team to be engaged. On the other hand, we need to change the management of the programs and to adapt patients expectations, realities, daily program. So we should focus on patients needs.
Host: That’s indeed a great lesson. And if we look ahead, what emerging area of exercise medicine, whether tele-rehabilitation, wearable devices or even AI excites you most?
Guest: Technology is an advantage nowadays. Tele-rehabilitation is a must is positive thing that we have. So it helps us solve the problem of access. Tele-rehabilitation can solve distance problem, time, capacity constraints. That means that we should focus on technology-based rehabilitation programs and also we should take into account that wearables should also help us. It is a means to monitor patients to record the habits, the heart rate responses, to also record sleep, recovery and symptoms and that means that we should definitely use wearables during our exercise training programs.
Host: Within this question, what do you envision the future of cardiac rehab in Greece?
Guest: We are a university cardiac rehab center. That means that we try to look forward. The opportunity is huge but still there are a lot of things to be done. We definitely have a lot of modalities, we have hybrid programs, we have tele-rehabilitation. It is important to solve many problems in Greece, first access and reimbursement. Unfortunately, the government doesn’t reimburse the exercise training sessions here in Greece. So, we are university and that’s why we managed to survive 35 years now. But the reality is not that positive actually. Also, we need to change the referral culture and we should also try to find different solutions for all patients. That’s why I believe that we need to have alternatives for all needs: center-based programs, home-based programs with technology, hybrid delivery, all kind of alternatives in order to increase participation. So I believe generally globally that personalized, hybrid and prevention-focused programs are the solution. So that means that we need to move towards home-based options towards digital options. And we should also focus on different aspects that mean that we should pay attention to mental health, to prevention, to cardiometabolic risk, to sleep, to patients quality of life and we should also include all kind of patient to have a broader eligibility.
Host: And within the scope of your research I’m curious to know if there are, when you think about cardiac rehab and expanding access, are there any special considerations for individuals with chronic kidney disease as well?
Guest: We try to copy everything we know from cardiac patients to any kind of other chronic diseases and that means that we should also transfer all the knowledge to chronic kidney disease patients. We started with center-based programs similar to what we did in cardiac patients. We found out that this was a bit difficult for them due to time restrictions. And then we changed the model. We offer intradialytic exercises. That means exercise during the dialysis sessions which is a model that can save time and that increases the participation rate. And then we also try to add technology in our programs. That’s why we deliver different kind of exercise training modality. We have hybrid, we also have wearables, we have technology. We added everything we know to the chronic kidney disease model. We know what the disadvantages are, what the differences are in the disease and we try to adapt our programs according to their needs, their capacities and their willingness.
Host: Oh, that’s impressive. Thank you. I have a more like a personal question. So, how do you balance the demands of research with teaching, mentorship or even a clinical practice?
Guest: A tough one. It requires structured time allocation. That’s the first: a schedule, also good partners, good team structure, a lot of trainees and also prioritizing things. I try to find trainees that are able to contribute and I try to increase the time – not only 24 hours a day – difficult task, but it works over time.
Host: Well, from a very successful woman in science and research. So thank you. Thank you for listening to Let’s Talk ICPR. Stay tuned for more episodes this season and don’t forget to subscribe to ICPR the Insider for the latest news, views and insights from our community.